Grothman Opens Roundtable on Examining Mental Health in the MAHA Age
WASHINGTON—Subcommittee on Health Care and Financial Services Chairman Glenn Grothman (R-Wis.) delivered opening remarks at today’s roundtable on “Examining Mental Health in the MAHA Age.” In his opening statement, Subcommittee Chairman Grothman highlighted that more Americans are seeking treatment for mental health issues than ever before, but that the outcomes of such treatment and the state of mental health today are significantly worse. He also pointed out that worsening mental health is harming the economy and causing the United States to lose billions in spending for programs that do not appear to be working.
Below are Subcommittee Chairman Grothman’s remarks as prepared for delivery:
Good afternoon, and welcome to the Subcommittee on Health Care and Financial Services’ first roundtable.
Today’s discussion will be a little different from a typical hearing. It will be more informal: we won’t be keeping strict time, and I encourage my colleagues to jump in with questions throughout. The goal is to have a candid conversation with the experts joining us today.
We are here to examine a difficult but urgent issue: the state of mental health in this country, why it appears to be getting worse, whether the system designed to address it is working, and what we in Congress should do about it.
Over the past two decades, the United States has dramatically expanded access to mental health care.
In 2002, about 27 million adults received mental health treatment. By 2024, that number had grown to nearly 60 million.
And yet, outcomes are moving in the wrong direction.
Depression rates are at historic highs. Suicide rates have climbed back to their highest levels in decades.
By multiple measures, Americans report worse mental health today than in previous generations.
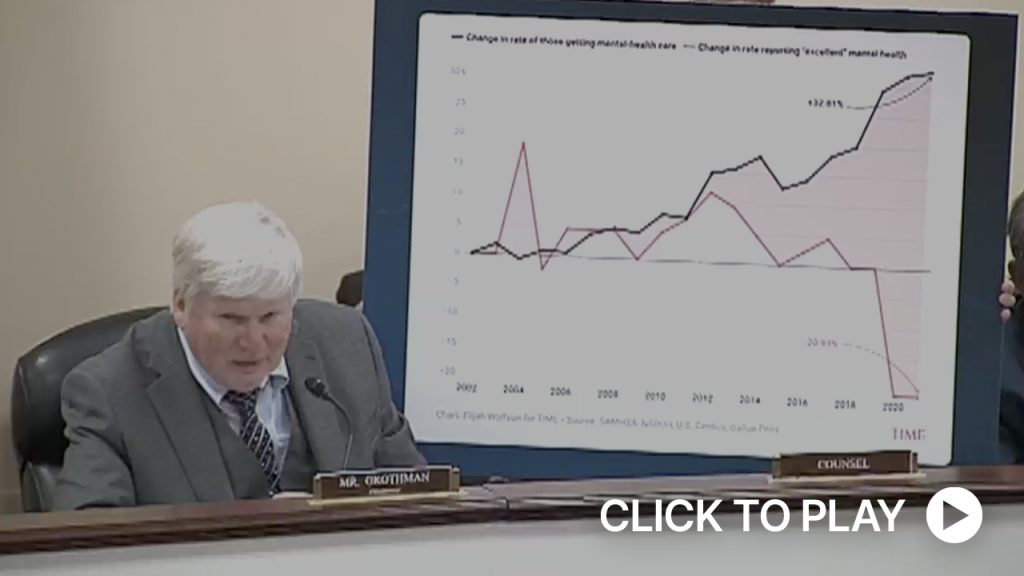
As you can see on the chart behind me, as individuals receiving mental health care increased, the rate at which they reported their mental health being excellent decreased.
That raises a fundamental question: if we are treating more people than ever before, why are we not seeing better results?
This is not just a public health concern—it is also an economic one.
A study published last week found that from 2000 through 2021, mental health and substance use disorders nominal spending grew from $40.9 billion to $139.6 billion. Mental health and substance use disorders accounted for 4.5 percent of all medical services spending in 2000 and 5.5 percent in 2021.
Real per capita mental health and substance use disorders spending grew at an average annual rate of 3.27 percent, which was faster than the growth rate for overall medical services which is 2.21 percent.
On the government spending side, more than one in three Social Security Disability Insurance beneficiaries are enrolled due to mental disorders, making it one of the largest drivers of a program originally intended for those with severe physical limitations.
At the same time, many Americans are bearing these costs personally. One in ten have gone into debt to pay for mental health care.
Perhaps most concerning is what we are seeing among young people.
Rates of mental health diagnoses in children and adolescents have risen sharply, along with the use of psychiatric medications.
Antidepressant prescriptions for individuals aged 12 to 25 increased by more than 63 percent between 2016 and 2022. During that time a total of more than 221 million antidepressants were prescribed and dispensed to 18 million individuals aged 12 to 25.
Yet even as treatment has expanded, outcomes for youth continue to worsen.
In 2021, 57 percent of teen girls reported persistent feelings of sadness or hopelessness, up from 36 percent just a decade earlier.
We are intervening more, medicating more, and spending more. Yet, many of the people we are trying to help are not getting better.
There is something in this system that is not working as intended.
Let me be clear about what today’s conversation is not.
This is not an argument against mental health care, nor is it an attempt to stigmatize those seeking help.
But when a system produces outcomes like these, despite significant investment, we have a responsibility to ask hard questions.
Recent efforts, including the Trump Administration MAHA Commission’s focus on over-medicalization and its direction to evaluate pediatric prescribing patterns, suggest that some of these questions are beginning to be taken seriously.
Our constituents already know something is wrong. They are living it. They are watching their children struggle, taking on debt for care, and searching for answers when the system falls short.
They deserve a system that works, and they deserve accountability when it does not.
That is what today’s roundtable is about.
I want to thank our witnesses for being here, and I look forward to a productive and honest discussion.
With that, I am now pleased to introduce our roundtable guests.
First, we have Dr. David Hyman. Dr. Hyman is an adjunct scholar at the Cato Institute and a Professor of Health Law & Policy at Georgetown Law.
Next, we have Dr. Sally Satel. Dr. Satel is a senior fellow at AEI, a practicing psychiatrist and a lecturer at the Yale University School of Medicine.
Next, we have Laura Delano. Ms. Delano is the founder of the Inner Compass initiative and is a leading voice in the international movement of people who’ve left behind the over medicalized and professionalized mental health industry to build something different.